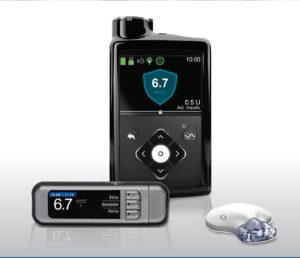
Introducing the MiniMed 670G with SmartGuard technology, the world’s first self-adjusting insulin pump system, reducing the burden of living with Type 1 diabetes. By Sue Marshall, editor, Desang Diabetes Magazine.
The MiniMed 670G system with SmartGuard Auto Mode is the world’s first self-adjusting insulin pump system. MiniMed 670G is a hybrid closed loop (HCL) insulin pump (it is called ‘Hybrid’ as some user interaction is required for carbohydrate entry and corrections). To put it simply, the new MiniMed 670G system when in SmartGuard Auto Mode automatically adjusts basal insulin every five minutes to meet the person individual needs. This helps reduce highs and lows and keep the person within a healthy glucose range.
Medtronic’s MiniMed 640G pump was launched in Europe nearly four years ago, having several hundred thousand users across Europe at present. Since then the company’s MiniMed 670G pump has been launched in the USA. Andrew Nicholson, EMEA Marketing Manager for Medtronic says, “The launch of the MiniMed 670G in the US has resulted in more than 100,000 people using the system to date. We have learnt so much from them and we are aware that this is a mindset shift for both people and their physicians. We are now very proud to have launched the MiniMed 670G system along with our new Guardian Sensor 3 in Europe. Early feedback has been very positive, and we are seeing excellent results.”
As we all know, for someone with diabetes it is extremely unlikely that any two days are alike treatment has to be adjusted not just daily but hourly, and simple things like exercise can be complicated to navigate. Dr Ohad Cohen, EMEA Medical Affairs Director for Medtronic, puts the new technology into perspective. He says, “To be honest this field in medicine has seen many changes since the discovery of insulin about 100 years ago. Today, people with diabetes can expect a full and healthy life. There are many reasons for this, including improvements in insulin formulations, advances in technology but also the attitude of the people with diabetes. People with diabetes are no longer passive but are participants in their own care. Their feedback and requests are driving things forward. But there apparently has been less progress in the recent 10 years.”
Significant change
It can also be said that there has been a significant change in the attitude of doctors too, with much more understanding and empathy in the diabetes sector compared even to a few decades ago. There has been a large amount of research done into diabetes care – or more exactly, diabetes self-care. Blood glucose seems to be infinitely measurable value, particularly in the form of HbA1c. For many a long year this number has been the sole goal of good control, yet HbA1c can only a rough guide, being a three-month aggregate of blood glucose levels. But in the absence of any other measure of diabetes control, it has been important.
Says Dr Cohen, “The fact is that 5.2% HbA1c is a normal HbA1c for a person without diabetes, yet control in Type I diabetes is rarely likely to get below 6.5%, and for many people that is unattainable. It is considered that 7% might be possible, but it’s still a compromise compared to a person without diabetes. Glucose is not the problem, it is actually the lack of insulin that is the problem. Insulin is a very difficult drug, as well as being dangerous. Give too much or too little and it’s wrong, you are either
too high or two low — it is a double-edged sword. Insulin itself does not know how and when to work.”
What this means in reality is that someone with diabetes has to be almost obsessive in order to be an ideal patient, constantly checking blood glucose and tweaking insulin doses all day long. “People with diabetes have to act like computers, taking many factors into account every day that can affect their control,” says Dr Cohen, “At Medtronic we knew we needed a solution that addressed both the highs and the lows. Time in range is therefore important. For a period HbA1c was all we had, but patients have been moving to make time in range a better way to judge diabetes control. The new aim is maximum time in range with minimum hypoglycaemia.”
Part of Medtronic’s approach was simply to make living with diabetes easier, meaning less work needing to be done by the person with diabetes, while at the same reducing the worry and risk of having hypos. It’s solution is SmartGuard technology, which is the name given to their closed loop technology. The latest development is SmartGuard Auto Mode, which now has FDA approval in the United States and CE Mark approval in Europe. Says Cohen, “We knew that a very important element in the treatment of Type 1 diabetes was to develop the algorithm needed to make a closed loop system.”
Closed loop means that, based on readings from the CGM sensor, the pump can be automated to deliver insulin when readings are high but also to suspend insulin delivery if readings are going low. “The algorithm that is inside the MiniMed 670G system has taken a decade to figure out,” says Cohen, “It has involved engineers with specialisms in applied mathematics and theoretical physics. This was no trivial maths problem.”
Reducing the burden
The MiniMed 670G system is the culmination of nearly 20 years of development, with many minds working together to tackle the problem of poor glycaemic control. The first sensor-augmented pump, Medtronic’s MiniMed 522, came out in 2006, then the Medtronic Paradigm VEO followed, which was able to ‘suspend on low’ using data from a CGM sensor. Medtronic launched the MiniMed 640G system with SmartGuard ‘suspend before low’ in 2015, which has since become the company’s main insulin pump being used in Europe. It works by predicting hypoglycaemia and has been proven to minimise the frequency of hypos, greatly reducing the user’s worries about having them.
David Dunleavy, an engineer with previous experience in the aerospace sector, is Senior Programme Director at Medtronic. He has been part of the team responsible for a closed loop program within Medtronic, and previously the low glucose suspend (LGS) feature in the MiniMed 640G. Dunleavy says, “These systems have put us on the path to reducing the burden of living with diabetes. The MiniMed 670G system’s automation of basal insulin delivery now puts us on the path towards the closed loop.”
At the moment the MiniMed 670G system is referred to as a hybrid closed loop insulin pump – hybrid as it does still need the user to input carbohydrate estimates and boluses. Having been available in the US for nearly two years, the MiniMed 670G system is now being launched globally, with the first countries in Europe — including the UK – having the product available only since November 2018.
Says Dunleavy, “You do have to work with the system — you get out what you put in, as with many things — but if you let it, the system works. It involves a bit of a leap of faith – for so long users have been encouraged to run their own diabetes, blood testing, carb-counting, bolusing. Diabetes is a very hands-on experience, and requires constant attention. The MiniMed 640G is both similar but different. With the MiniMed 670G you have to take direction from the system as it will tell you to test your blood glucose and when to calibrate, and on occasion it will suggest that you do a bolus. The best thing you can do, is to do what it tells you to, and don’t do anything beyond that. Understandably, it is hard to give over control to a bit of technology, but it does adapt to you and to your version of diabetes. Don’t try and second-guess it. You have to trust it and take your hands off the wheel a bit.”
Work experience
So how does it work? The components of the system are: The all new Guardian Sensor 3 glucose sensor, the Guardian Link 3 transmitter; an infusion set; a blood glucose meter; Carelink software, insulin-to-carb ratio; and the MiniMed 670G pump with SmartGuard technology.
Simple things are set up in the pump at the start by the user, under the care of a healthcare professional, including the person’s insulin-to-carb ratio and active insulin time. Then there is a three-day period where the pump is on the person but the SmartGuard Auto Mode is off (it reverts back to the same functionality as the MiniMed 640G system).
Once SmartGuard Auto Mode is turned on, a reading is taken every five minutes by the Guardian Sensor 3 CGM sensor. Based on this the dynamic SmartGuard Auto Mode algorithm in the pump makes changes to the user’s basal rate, adjusting either up or down in order to keep the glucose level stable. Every 24 hours at midnight the pump resets based on what has happened on the previous day.
Speaking further about the MiniMed 670G system, Medtronic’s EMEA Marketing Manager Andrew Nicholson says, “This is cutting-edge technology delivers improved glycaemic control whilst allowing the person to hopefully think less about their diabetes. With the MiniMed 640G system the focus had been on preventing lows; with the MiniMed 670G we are addressing the highs as well as lows. When in SmartGuard Auto Mode, the system adjusts to the persons real time glucose needs by giving small amounts of basal insulin every five minutes as the system target a glucose level of 6.7 mmol/L.
All the range
Referring back to time in range (TIR), this is a more modern way of measuring diabetes control, made possible in the main by the evidence supplied by the use of CGM sensors and expressed as a percentage: the percentage of time someone with diabetes spends within the optimal range of above 3.9 mmol/L and under 10 Mmol/L. Studies have shown that people using multiple daily injections (MDI) spend on average 45% of their time in range. It has to be noted that these studies tend to be based on people with diabetes who have fairly good control, so others on MDI might not achieve that number. Those using an insulin pump have been shown as having 51% time in range, and those using a sensor-and-pump combination achieving an average of 57% time in range.
Says Cohen, “We think you deserve better than this. We are trying to move people to better control by improving time in range as well as HbA1c. The way you run your diabetes currently takes a lot of effort, don’t underestimate how much you know, and how much it is that you do to control your diabetes. Our hope is that you will have to think less about your diabetes. Time in range is a more modern metric, thanks to the increased use of CGM sensors over recent years. It’s really about time in ‘ranges’ – less time low, less time high, more time in the middle. The great news is that users of the MiniMed 670G system in clinical trials in the US have been proven to be spend an average of 72% time in range. Our hope is to get the amount of time spent in range even higher than that.”
News items and features like this appear in the Desang Diabetes Magazine, our free-to-receive digital journal (see below). We cover diabetes news, diabetes management equipment (diabetes ‘kit’ such as insulin pumps and continuous glucose monitoring equipment) and news about food suitable for a diabetic diet including a regular Making Carbs Count column. We just need your email address to subscribe you (it’s free, and you can easily unsubscribe should you wish to).